Pharmacogenomics, a branch of pharmacology, studies the effects of variations in genetic makeup on the response of drugs and medicine. Combining traditional pharmaceutical sciences with knowledge of genes, proteins, and single nucleotide polymorphisms, pharmacogenomics is a promising field that one day may lead to drugs which are custom-made for individuals and adapted to each person's own genetic makeup. A lot of factors can influence a person's response to medicine, but it is thought that the most effective way to create personalized drugs is through individuals genetic makeup. Though the practical use of pharmacogenomics in medicine is still in its early stages, the prospect of personalized medicine is a popular and emerging idea.
Drug Metabolism
It is possible for genetic variations to cause problems in producing active forms of enzymes. If a drug relies on these enzymes to metabolize them, then giving that drug to a person with that genetic variation could be very dangerous. Drug overdose may result from the enzyme's inability to eliminate that drug from the body. It's important to test for these sort of DNA variations so the drug dosage can be administered correctly.
Cytochrome P450 One of the most studied proteins in pharmacogenomics is the cytochrome P450 (CYP) family of liver enzymes. These enzymes are responsible for breaking down more than 30 different classes of drugs. DNA variations in the genes that code for these enzymes can influence their ability to metabolize certain drugs. (78) If a patient has inactive or less active forms of CYP enzymes, they may be unable to break down and proficiently remove drugs from the body, causing a drug overdose. Today, clinical trial researchers use genetic sequencing technologies to test for variations in the CYP genes, to screen and monitor patients. (78) Thiopurinemethyltransferase Thiopurinemethyltransferase (TPMT) is another enzyme which breaks down a class of therapeutic compounds called thiopurines. This enzyme is really important in the chemotherapy treatment of a common childhood leukemia disease. If a patient had inactive forms of TMPT, they would be unable to break down thiopurines and the drug will elevate to toxic levels. A small percent of Caucasians have a genetic variation which prevents an active form of this protein from being produced. Because of this possibility, nowadays doctors use a genetic test to screen for this deficiency, and the appropriate measures are taken to keep the thiopurine levels at safe amounts. (78) | 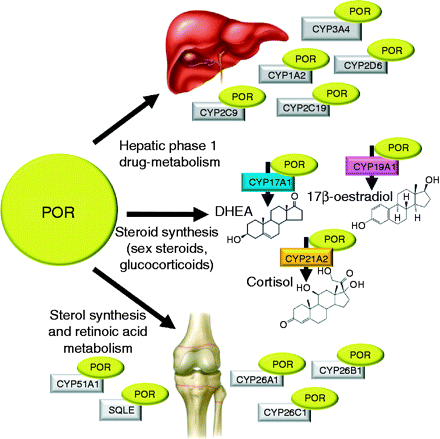 Figure (79) |
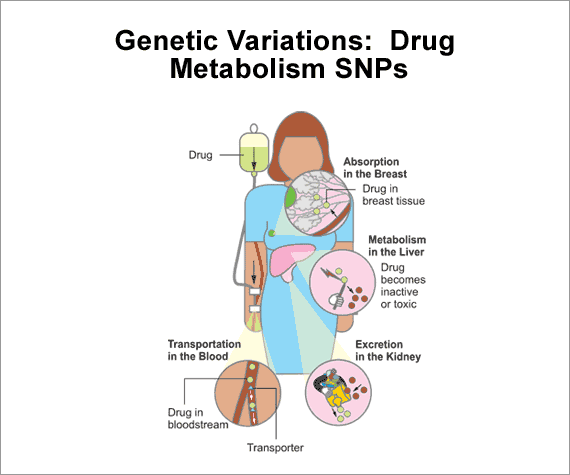
When a person takes medication, many proteins in his or her body interact with the drug as it is transported throughout the body, absorbed into tissues, metabolized into more active forms or toxic byproducts, and excreted. If an individual has SNPs (single nucleotide polymorphisms) in any one or more of these proteins, they may alter the time the body is exposed to active forms of a drug or to any of its toxic byproducts. Text and Figure (80)
|  |
